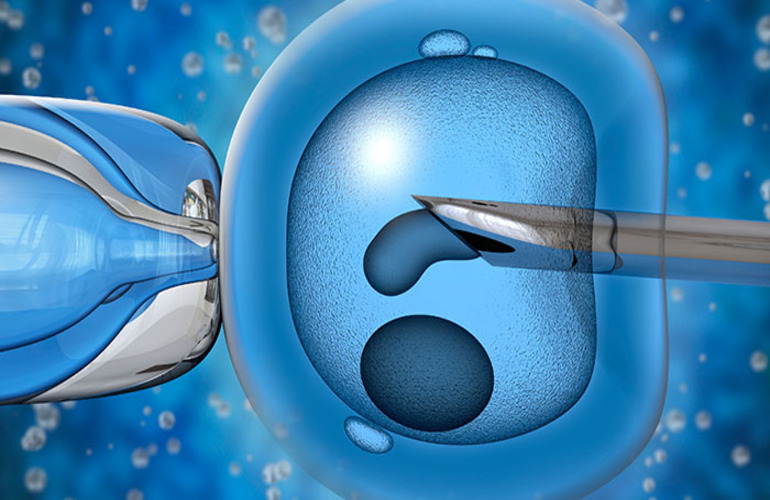
What Is Egg Quality and Why It Matters in IVF
Egg Quality is a critical factor in determining the success of in vitro fertilization (IVF) procedures. It refers to the health and viability of a woman’s eggs, which are essential for successful fertilization and proper embryo development. High-quality eggs increase the likelihood of achieving a healthy pregnancy by supporting the growth and implantation of a viable embryo.
Factors influencing Egg Quality include the maturity of the egg, its genetic integrity, and overall cellular health. Understanding the role of Egg Quality is crucial for women undergoing IVF, as it directly impacts the chances of conception and the outcome of fertility treatments.
Reproductive specialists highlight the importance of Egg Quality when tailoring personalized IVF plans. By incorporating lifestyle modifications, nutritional strategies, and medical interventions aimed at improving Egg Quality, women can enhance their chances of a successful IVF journey. Taking proactive steps to focus on this key factor can make a significant difference in achieving a positive fertility outcome.
Factors Affecting Egg Quality in Women
Egg quality is influenced by a variety of factors that can impact a woman’s reproductive health and her chances of successful conception through methods like IVF. Understanding these factors is crucial for those considering fertility treatments and can help in making informed decisions regarding their reproductive health.
Age
As women age, the quality and quantity of their eggs decline. This natural process can affect not only the chances of conception but also the success rates of assisted reproductive technologies. Women are born with a finite number of eggs, and over time, both the eggs and their cellular environment become less robust.
Genetics
Genetic factors play a significant role in determining egg quality. Chromosomal abnormalities in eggs can lead to issues during fertilization and embryo development. Women with a family history of fertility challenges may also experience similar difficulties, further underscoring the impact of genetics on egg quality.
Lifestyle Choices
Certain lifestyle choices significantly affect egg quality. Factors such as smoking, excessive alcohol consumption, and drug use have been shown to negatively correlate with fertility. Moreover, maintaining a healthy weight is also important, as both overweight and underweight conditions can disrupt hormonal balance and affect ovulation.
Environmental Factors
Exposure to environmental toxins, such as pesticides, heavy metals, and endocrine disruptors, can adversely affect egg quality. Women who work in industries with high exposure to chemicals may want to consider lifestyle adjustments to minimize contact with harmful substances.
Hormonal Balance
The hormonal environment within a woman’s body is pivotal for optimal egg quality. Conditions such as polycystic ovary syndrome (PCOS) or thyroid imbalances can hinder hormone production and disrupt ovulation, thereby compromising egg quality. Regular hormone level checks can help in diagnosing and managing such conditions.
Several interconnected factors contribute to egg quality in women, influencing their fertility potential and overall reproductive health. Understanding these factors can empower women to take proactive measures, whether through lifestyle changes or medical intervention, to enhance their egg quality.
How to Assess Your Egg Quality Before IVF
Assessing your egg quality before undergoing IVF is a critical step in the journey towards conception. Since egg quality can significantly influence the success of IVF procedures, understanding how to evaluate it can empower women to make informed decisions. Here are the most effective methods for assessing your egg quality:
1. Hormonal Testing: Blood tests can measure hormone levels such as Follicle Stimulating Hormone (FSH), Luteinizing Hormone (LH), and Estradiol on specific days of your menstrual cycle. Elevated FSH levels may indicate decreased ovarian reserve and egg quality.
2. Antral Follicle Count (AFC): This ultrasound test, conducted early in your menstrual cycle, counts the number of small follicles in the ovaries. A higher count typically suggests better egg quality and quantity.
3. Ovarian Reserve Testing: Tests like the Anti-Müllerian Hormone (AMH) level can provide insight into the health and quantity of eggs in the ovaries. Low AMH levels may correlate with lower egg quality.
4. Genetic Testing: Preimplantation Genetic Testing (PGT) through IVF can be performed to analyze the chromosomes of embryos before transfer. This can help assess the genetic viability of eggs and embryos created from them.
5. Lifestyle Assessment: Evaluating factors such as smoking, alcohol consumption, diet, and weight can provide clues about egg quality. Implementing lifestyle changes can potentially enhance your reproductive health.
6. Consult a Fertility Specialist: Speaking with a fertility expert can provide personalized insights based on your medical history, test results, and overall health. They may recommend additional assessments tailored to your needs.
By taking these steps, you can gain a clearer understanding of your egg quality. This knowledge not only helps in preparing for IVF but also allows you to make individualized lifestyle or medical adaptations aimed at enhancing your chances of success.
The Impact of Age on Egg Quality and IVF Success
Age is one of the most significant factors affecting egg quality, which in turn influences the success rates of in vitro fertilization (IVF). As women age, the quantity and quality of their eggs decline, primarily due to the natural aging process of the ovaries. This decline affects various aspects of fertility, including the ability to conceive, the likelihood of implantation, and the overall success of IVF procedures.
Research indicates that women are born with a finite number of eggs, which diminishes over time. By the late 20s to early 30s, fertility begins to decline slowly, but the rate accelerates significantly after age 35. Specifically, by age 40, many women experience a sharp decline in both the number of viable eggs and the quality of those eggs, making conception increasingly challenging.
Egg quality refers to the health and maturity of the eggs; lower quality eggs are more likely to lead to chromosomal abnormalities, which can result in failed implantation, miscarriage, or other complications during early pregnancy. As a result, women over the age of 35 often face lower success rates with IVF, making early intervention essential for those seeking to conceive.
Moreover, the impact of age on egg quality is not uniform across all women. While some may experience a steep decline in fertility, others may find they can conceive later in life. Factors such as genetics, lifestyle choices, and overall health also play critical roles in determining egg quality at different ages.
In IVF treatment plans, specialists often consider a woman’s age during assessments and recommend individualized approaches to improve outcomes. This may involve lifestyle modifications, ovarian reserve testing, and sometimes the consideration of egg donation as an option for those with significantly reduced egg quality.
Understanding the link between age and egg quality is vital for women planning their families, especially as societal trends move towards later motherhood. Being informed about the implications of age can empower women to make choices that align with their reproductive goals.
Understanding Egg Quality Testing for IVF Candidates
When preparing for in vitro fertilization (IVF), understanding egg quality testing is crucial for candidates seeking successful outcomes. The quality of eggs can significantly affect the chances of conception and the health of the embryo. Various tests are available to help assess egg quality, empowering individuals to make informed decisions regarding their reproductive health.
Types of Egg Quality Testing
There are several methods to evaluate egg quality, including:
- Hormonal Analysis: Blood tests can measure levels of hormones like FSH (Follicle-Stimulating Hormone), LH (Luteinizing Hormone), and estradiol, which provide insights into ovarian reserve and egg quality.
- Ultrasound Imaging: A transvaginal ultrasound can visualize the ovaries and follicles, allowing physicians to assess the developmental stages of eggs and the overall ovarian response.
- Genetic Testing: Preimplantation genetic testing (PGT) can be performed on embryos created through IVF to evaluate their genetic health, indirectly indicating the quality of the eggs used.
Interpreting Test Results
Interpreting these test results requires professional guidance. A fertility specialist will analyze the findings and may suggest further testing or treatment options based on the individual circumstances. For instance, a high level of FSH may suggest diminished egg quality, while a healthy follicle count observed through ultrasound can indicate a good ovarian response.
Steps to Take After Testing
Once egg quality testing is completed, it is essential to take actionable steps. Based on your results, consider discussing the following with your healthcare provider:
- Possible lifestyle changes to improve overall health and egg quality.
- Nutritional strategies tailored to support reproductive health.
- Consideration of advanced reproductive technologies based on egg quality findings.
Being well-informed about egg quality and the testing processes can empower IVF candidates to navigate their journeys with greater confidence, making choices that enhance their chances for a successful pregnancy.