An Overview of Uterine Adhesions: What is Asherman Syndrome?
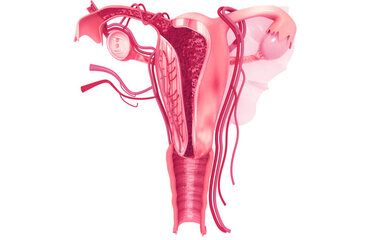
Asherman Syndrome is a medical condition defined by the formation of scar tissue or adhesions within the uterine cavity. These adhesions typically develop after surgical procedures like dilation and curettage (D&C), cesarean sections, or other uterine surgeries. The condition can lead to menstrual irregularities, infertility, and other complications, depending on the severity of the adhesions.
Symptoms of Asherman Syndrome vary widely. Some women experience mild disruptions, while others face significant challenges such as severe menstrual pain or the inability to conceive. The presence of these adhesions can hinder the uterus’s normal function, impacting reproductive health and overall well-being.
Common Warning Signs and Diagnostic Tools
The symptoms of uterine adhesions are not always immediately noticeable, making diagnosis challenging. Here are some indications that may prompt further investigation:
- Menstrual Changes: Irregular, light, or absent periods are common signs.
- Pelvic Pain: Pain during menstruation or in daily life can signal adhesions.
- Fertility Challenges: Difficulty conceiving or repeated miscarriages may indicate a structural issue within the uterus.
To diagnose the condition, healthcare providers use a combination of techniques such as transvaginal ultrasound, hysterosalpingography (HSG), and hysteroscopy. These methods provide insights into the uterine cavity’s structure and the extent of any adhesions present.
Risk Factors and Potential Causes
The development of uterine adhesions often stems from past medical or surgical events. Key factors include:
- Previous Surgeries: Procedures like D&C or cesarean sections are common contributors.
- Infections: Postpartum infections or pelvic inflammatory conditions can lead to scarring.
- Endometrial Trauma: Injuries to the uterine lining, particularly following pregnancy complications, increase risk.
- Other Factors: Radiation therapy or congenital uterine abnormalities may also play a role.
Understanding these risks is crucial for prevention and early intervention.
Treatment Approaches to Improve Outcomes
Managing uterine adhesions involves both surgical and non-surgical options. A common approach is hysteroscopic surgery, a minimally invasive method to remove scar tissue and restore the uterus’s normal function. Post-surgical care may include hormonal therapy to encourage healing and prevent recurrence.
In addition to medical treatments, follow-up care is vital. Patients may undergo imaging studies or use temporary devices to maintain uterine structure and reduce the risk of further adhesions. Emotional support through counseling or support groups can also aid in the recovery process.
Long-Term Considerations for Reproductive Health
Untreated uterine adhesions can have significant implications, particularly for fertility and pregnancy. These include:
- Infertility: Adhesions can block fallopian tubes or interfere with implantation.
- Pregnancy Complications: Risks such as miscarriage or abnormal placental attachment increase.
- Menstrual Irregularities: Persistent changes in cycle regularity can affect overall health.
By addressing these issues early, women can improve their chances of successful pregnancies and minimize long-term effects.
Steps for Women Facing Uterine Adhesion Challenges
For women navigating life with uterine adhesions, proactive care and informed decision-making are key. Consider the following:
- Stay Informed: Learn about the condition and its potential impacts.
- Consult Specialists: Seek advice from reproductive health experts for accurate diagnosis and tailored treatments.
- Follow Treatment Plans: Adhere to recommended medical and surgical interventions to improve outcomes.
- Build a Support Network: Engage with others who have similar experiences to share strategies and emotional support.
Taking these steps can empower women to manage their health effectively and achieve their reproductive goals.